The Ultimate Guide to How to Stop Bedwetting Fast: Everything You Need to Succeed in 2026

Welcome to 2026, where the days of "waiting it out" and waking up to soggy sheets are officially a thing of the past! If you’re a parent navigating the exhausted, laundry-filled trenches of nighttime accidents, take a deep breath. You aren’t just looking for a "fix", you’re looking for a victory.
At Elevacare Health LLC, DBA Bladder Breakthrough, we believe every child has a superhero inside them waiting to be awakened. Bedwetting (medically known as nocturnal enuresis) isn't a behavioral flaw, a sign of laziness, or a "phase" you have to suffer through silently. It’s simply a communication gap between the brain and the bladder.
In this ultimate 2026 guide, we are going to bridge that gap using the latest science, pediatric pelvic floor techniques, and the magic of gamified therapy. Get ready to join the Stay Dry Squad™. It’s time to level up!
The 2026 Shift: Why "Wait and See" is History
For decades, the standard medical advice was: "Don't worry, they'll outgrow it." While it’s true that many children eventually stop bedwetting, the emotional toll of waiting can be massive. By 2026, the pediatric community has shifted. We now know that early, proactive intervention, focused on the brain-bladder connection, leads to faster results and higher self-esteem for the child.
Bedwetting in children affects roughly 15% of five-year-olds and 10% of seven-year-olds [1]. But here’s the kicker: those aren’t just numbers. Those are kids missing out on sleepovers, parents losing sleep, and families feeling the weight of a "secret" struggle.
We don't wait for the body to "figure it out" anymore. We train it. We use bladder training for kids that feels like a game, not a chore.

(Image Description: A diverse, heroic family, mom, dad, and their son, wearing colorful superhero capes, standing together in a brightly lit living room. They are looking at a tablet together with high-fives and big smiles, celebrating a digital trophy on the screen. The vibe is triumphant and unified.)
The Science of the Soggy Sheet: What’s Actually Happening?
Before we get to the "how-to," we have to understand the "why." Bedwetting is rarely caused by one single thing. It’s usually a "Perfect Storm" of three factors:
- The Heavy Sleeper Syndrome: The brain simply doesn’t receive the "I’m full!" signal from the bladder while the child is in a deep sleep state.
- Overproduction of Midnight Oil: Some kids don't produce enough ADH (antidiuretic hormone) at night, meaning their kidneys keep pumping out urine at daytime volumes [3].
- The Tiny But Mighty Bladder: Sometimes the bladder has a functional capacity that is smaller than the volume of urine produced overnight.
The Brain-Bladder Comm-Link
Think of the brain and the bladder like two superheroes on a mission. The bladder is the "Base," and the brain is "Command Center." In kids who wet the bed, the "comm-link" is fuzzy. Our goal with nighttime potty training in 2026 is to clear the static and strengthen that signal.
Step 1: Rule Out the "Hidden Villains"
Before starting any program, we must clear the field of obstacles.
The Constipation Connection
Did you know that the #1 hidden cause of bedwetting is actually... poop? It’s true! When a child is even slightly constipated, the rectum sits right against the bladder. A full rectum puts pressure on the bladder, making it twitchy and reducing its capacity. You cannot fix a bladder issue without fixing a bowel issue.
Sleep Apnea and Airway Issues
If your child snores like a freight train, their bedwetting might be linked to their breathing. When the body struggles for air, it creates a pressure change in the heart that signals the kidneys to produce more urine.
Step 2: Superpower Training (Pediatric Pelvic Floor Exercises)
This is where the Bladder Breakthrough method shines. Most people think pelvic floor exercises are just for adults, but kids have those muscles too! These muscles are the "brakes" of the bladder.
By teaching your child pediatric pelvic floor exercises, you are giving them the physical tools to hold on when that midnight signal finally breaks through.
- The Bladder Bounce™: A fun way to engage the core and pelvic floor while jumping (safely!).
- Elevator Ups: Visualizing the pelvic floor as an elevator going up to the "penthouse" and holding it there.
You can dive deeper into these techniques through our Theraplay: Empowering Kids Through Playful Bladder Support module.
Step 3: Gamification – The "Secret Sauce" of 2026
Let’s be real: no kid wants to do "medical exercises." But every kid wants to "Level Up."
This is why we created the Stay-Dri Eduplay™ universe. By turning the journey into a quest, we remove the shame and replace it with dopamine. When a child uses the Bladder Defender Gaming App, they aren't "fixing a problem", they are training their avatar to save the kingdom.
> "Gamification isn't just a trend; it's a neurological hack. By associating bladder signals with rewards and play, we accelerate the brain's ability to prioritize those signals during sleep." , Dr. Tiffani S. Bacon, PT

(Image Description: A stylized, futuristic 3D illustration of the brain-bladder connection. The brain is depicted as a glowing "Command Center" sending a bright blue lightning-bolt signal down to a "Base" (the bladder). The image looks like a high-tech video game interface.)
The Ultimate "Stop Bedwetting Fast" Blueprint
If you want to see results in weeks, not years, follow this 2026 Battle Plan:
1. The Daytime Hydration Strategy
Don't make the mistake of dehydrating your child! If they don't drink during the day, their bladder never learns how to stretch.
- The 70/30 Rule: Have your child drink 70% of their daily water before 4:00 PM.
- Limit "Bladder Irritants": Cut out caffeine (sodas), excessive sugar, and artificial dyes in the evening, as these can irritate the bladder lining [2].
2. Double Voiding
Make "Peeing Twice" the new bedtime standard.
- Pee at the start of the bedtime routine.
- Pee again right before the head hits the pillow.
- This ensures the "Base" is as empty as possible before the mission starts.
3. Use the Tech Sidekick (Urine Alarms)
Research shows that behavior therapy with a urine alarm is the gold standard for long-term success [1]. In 2026, these aren't the clunky buzzers of the past. They are sleek, smart, and integrate with apps like our Bladder Bounce App Tracker.
- How it works: The second a drop of moisture is detected, the alarm sounds. This "startles" the brain into recognizing the bladder signal.
- The "Overlearning" Phase: Once they are dry for 14 nights, we actually have them drink a little water before bed while keeping the alarm on. This "stress tests" their new skills to prevent relapse [1].
4. Positive Reinforcement ONLY
Shame is the enemy of progress. In the Stay Dry Squad, we celebrate the effort, not just the dryness.
- Did they help change the sheets? Victory!
- Did they remember their "Elevator Up" exercises? Level Up!
- Check out our Bladder Breakthrough Celebration for ideas on how to reward these wins.
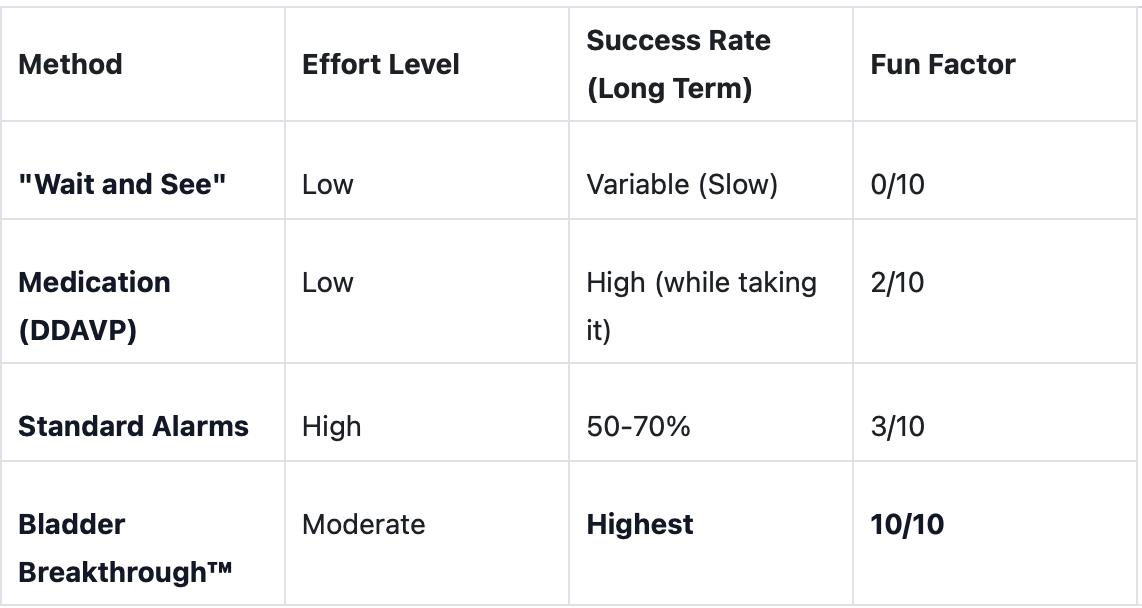
Comparing the Options: Why Digital Therapy Wins
Medications like Desmopressin can be a great "patch" for sleepovers or camp [4], but they rarely solve the underlying issue. When the pills stop, the wetting often returns [1]. Our Stay Dri Master Plan focuses on permanent, functional change.
A Note from the Front Lines: You Are Not Alone
I’ve seen thousands of families walk this path. The frustration you feel is valid. The exhaustion is real. But I want you to imagine a morning three months from now. You walk into your child's room. The air is fresh. The sheets are dry. Your child is beaming with a level of confidence you haven't seen in years.
That isn't just a dream, it’s the reality for families who commit to the process. Whether you start with our 5-Day Bladder Breakthrough Challenge or jump straight into the Virtual Course, the first step is deciding that "good enough" isn't good enough anymore.

(Image Description: A young girl of South Asian descent standing on her bed in her pajamas, holding a "Gold Trophy" made of cardboard, looking like a victorious superhero. Her father, an African American man, is cheering in the background. The room is decorated with "Stay Dry Squad" posters.)
2026 Bedwetting FAQ Insights
Q: How do I stop bedwetting fast in 2026?
A: The fastest way to stop bedwetting is a multi-modal approach combining pediatric pelvic floor exercises, gamified behavioral tracking, and a smart urine alarm. Using a system like the Bladder Breakthrough™ helps retrain the brain-bladder connection more efficiently than traditional methods.
Q: Is there a cure for bedwetting in 7-year-olds?
A: While "cure" is a strong word, most nocturnal enuresis can be successfully managed and resolved through behavioral modification and addressing underlying factors like constipation and sleep hygiene.
Q: What are the best pelvic floor exercises for kids?
A: Exercises like "Elevator Ups" (pelvic floor lifts) and the "Bladder Bounce™" (core engagement) are highly effective. These should always be taught in a fun, non-medicalized way to ensure compliance.
Q: Does the Bladder Defender app really work?
A: Yes! By utilizing "edutainment," the Bladder Defender app keeps kids engaged in their therapy, which research shows significantly improves outcomes compared to standard clinical instructions.
Q: Where can I find a pediatric pelvic floor physical therapist?
A: You can access specialized care through digital therapy platforms like Bladder Breakthrough, which offers virtual courses and gamified support systems designed by experts like Dr. Tiffani S. Bacon, PT.
References & Further Reading
- Caldwell PH, et al. (2020). Bedwetting and behavioral alarms: A systematic review of long-term outcomes. Journal of Pediatric Urology.
- National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK). (2023). Symptoms & Causes of Bedwetting.
- Neveus T. (2017). Pathophysiology of nocturnal enuresis. Handbook of Clinical Neurology.
- American Academy of Pediatrics (AAP). (2025). Clinical Practice Guidelines for Nocturnal Enuresis Management.
- Bacon, T. S. (2026). The Gamification of Pediatric Pelvic Health: A New Era of Intervention. Elevacare Health White Paper.
Ready to join the squad?
Don't let another night go by in the "Soggy Zone." Check out our Price Comparison to find the right level of support for your family.
Let’s do this. Together. 🚀💦🚫

(Image Description: A close-up of a "Super Hero" badge that says "Certified Stay Dry Squad Member" pinned to a child's pajama top. The child’s hand is giving a "thumbs up" next to it.)
Disclaimer: This guide is for educational purposes and does not replace professional medical advice. Always consult with your pediatrician to rule out underlying medical conditions. See our Legal & Privacy Terms for more information.